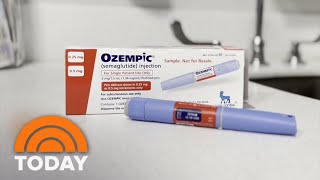
Semaglutide Safety Concerns: FDA's Latest Warning
The FDA has issued a warning to Novo Nordisk regarding potential unreported side effects and deaths linked to Ozempic, a semaglutide-based medication. This article delves into the implications for patients, healthcare providers, and the pharmaceutical industry, providing a comprehensive analysis of the situation.

Introduction
The FDA has recently issued a warning to Novo Nordisk concerning potential unreported side effects and deaths associated with Ozempic, a medication containing semaglutide. This development is significant as it raises questions about drug safety protocols and the responsibilities of pharmaceutical companies.
Background/Context
Semaglutide is a GLP-1 receptor agonist used primarily in the treatment of type 2 diabetes and obesity. Approved by the FDA in 2017, Ozempic has been widely prescribed due to its efficacy in controlling blood sugar levels and aiding weight loss. The drug represents a significant advancement in diabetes management, but its possible side effects have been a concern since its introduction.
According to data from the American Diabetes Association, GLP-1 receptor agonists can cause side effects ranging from gastrointestinal issues to more severe complications like pancreatitis. The FDA's warning highlights the need for ongoing vigilance in monitoring these medications.
Current Situation
As of now, the FDA's warning to Novo Nordisk underscores potential gaps in the reporting of adverse effects related to Ozempic. The agency has stressed the importance of accurate and timely reporting to ensure patient safety and maintain trust in pharmaceutical products. Industry sources indicate that unreported side effects could range from mild to severe, including rare cases of fatalities.
Healthcare providers are being advised to closely monitor patients on semaglutide and report any adverse events to the FDA's MedWatch program. This heightened scrutiny is crucial for identifying patterns that could lead to further investigations or changes in drug labeling.
Deep Analysis
The underlying causes of the FDA's warning can be traced to several factors. Firstly, the competitive landscape of diabetes medications has led to aggressive marketing strategies, which may prioritize sales over comprehensive safety reporting. Secondly, the complexity of pharmacovigilance (the process of monitoring the effects of medical drugs) can lead to discrepancies in data collection and reporting.
Stakeholder dynamics, including the roles of pharmaceutical companies, regulatory bodies, and healthcare providers, are central to ensuring drug safety. The FDA's warning serves as a reminder of the critical balance between innovation and regulation in the pharmaceutical industry.
Impact/Outlook
In the short term, the FDA's warning may lead to increased scrutiny of Novo Nordisk's pharmacovigilance practices. If further issues are identified, this could result in regulatory actions such as fines or restrictions on marketing. For patients, this means a potential re-evaluation of the risks and benefits of continuing Ozempic therapy.
Long-term, this situation could prompt a broader review of safety protocols for GLP-1 receptor agonists, potentially influencing future drug approvals and monitoring practices. The pharmaceutical industry may also face increased pressure to enhance transparency and accuracy in adverse event reporting.
Practical Implications
For healthcare providers, this situation emphasizes the importance of vigilant monitoring and reporting of side effects. Patients should be encouraged to report any unusual symptoms promptly. Pharmaceutical companies must prioritize pharmacovigilance to maintain trust and ensure patient safety.
Regulators might consider revising guidelines to strengthen the reporting framework, ensuring that all stakeholders are aligned in their efforts to protect public health.
Key Takeaways
- The FDA has warned Novo Nordisk about potential unreported side effects of Ozempic.
- Semaglutide, used for diabetes and obesity, is under scrutiny for safety concerns.
- Pharmacovigilance practices are critical in protecting patient safety and trust.
- Healthcare providers should closely monitor and report adverse events.
- Future regulatory actions could impact the pharmaceutical industry significantly.
- Enhanced transparency and accuracy in reporting are essential for drug safety.